Autoimmune Diseases: What You Need to Know
If your immune system is supposed to protect you, why does it sometimes turn against your own body? That’s the core problem with autoimmune diseases. Millions of people live with conditions where the body attacks itself, causing pain, fatigue and a range of other issues. The good news is that doctors now have better tools to diagnose and treat these disorders, and lifestyle changes can make a big difference.
Common Symptoms & Signs
Autoimmune diseases don’t all look the same, but they share some red flags. Persistent fatigue that doesn’t improve with rest is a classic sign. Joint pain or swelling, especially in hands and knees, often points to rheumatoid arthritis or lupus. Skin rashes that come and go, like the butterfly rash on the face, are another clue.
Digestive problems such as chronic diarrhea or abdominal pain can be linked to celiac disease or Crohn’s disease—both autoimmune. If you notice unexplained weight loss, fever, or a general feeling of being unwell for weeks at a time, it’s worth talking to a doctor about possible autoimmunity.
Because symptoms overlap with many other conditions, doctors use blood tests that look for specific antibodies. Tests like ANA (antinuclear antibody) can help pinpoint the disorder. Early detection means treatment can start sooner and prevent long‑term damage.
Managing Autoimmune Conditions
Treatment usually combines medication and lifestyle tweaks. Anti‑inflammatory drugs such as NSAIDs can ease pain, while disease‑modifying agents like methotrexate slow the immune attack. Newer biologic therapies target specific parts of the immune system and have changed outcomes for diseases like psoriasis and multiple sclerosis.
Beyond prescriptions, diet plays a big role. Many patients find relief by cutting out gluten, dairy or processed sugars—foods that can trigger inflammation. A Mediterranean‑style eating plan rich in fish, olive oil, fruits and vegetables supports overall immune health.
Regular gentle exercise helps keep joints flexible and reduces fatigue. Even short walks or yoga sessions can boost mood and improve sleep, which is crucial because poor rest often worsens symptoms.
Stress management is another pillar. Chronic stress spikes cortisol, a hormone that can aggravate autoimmunity. Simple practices like deep breathing, meditation or spending time outdoors can keep stress levels in check.
If you’re looking for reliable information on specific drugs or want to compare treatment options, Sevencells Pharmaceuticals offers detailed articles on medications such as Femara, Forxiga and many others. Check out our guides to learn where to buy safely online and what side effects to watch for.
Living with an autoimmune disease is a daily balancing act, but understanding the condition, staying on top of medical care, and making smart lifestyle choices can dramatically improve quality of life. If you suspect something’s off, schedule a visit with your healthcare provider—early action makes all the difference.
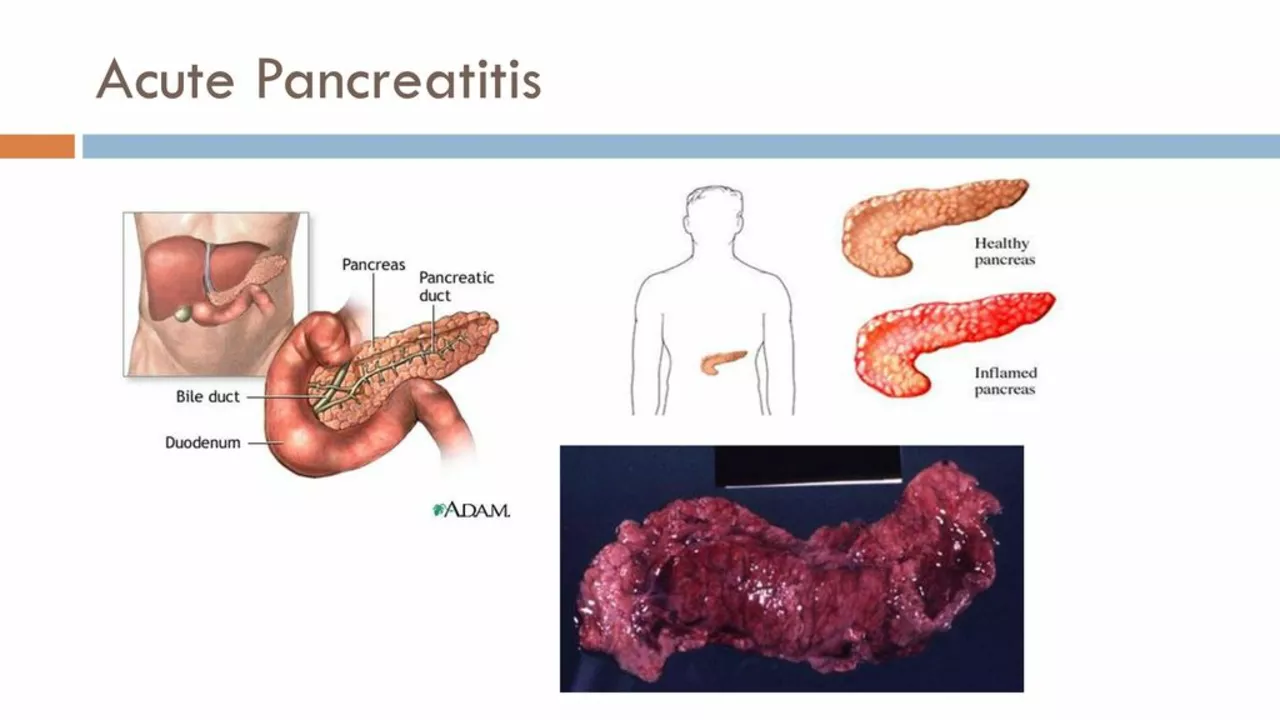
The Connection between Pancreatic Duct Blockage and Autoimmune Diseases
In a recent study, I found a fascinating connection between pancreatic duct blockage and autoimmune diseases. The blockage in the pancreatic duct can lead to inflammation, which may trigger the immune system to attack the body's own tissues. This, in turn, can result in the development of autoimmune diseases like type 1 diabetes, celiac disease, and lupus. It's crucial to recognize these connections to find better treatment and prevention strategies for people suffering from these conditions. As a blogger, I am committed to raising awareness on this topic and promoting further research to improve the lives of those affected by autoimmune diseases.